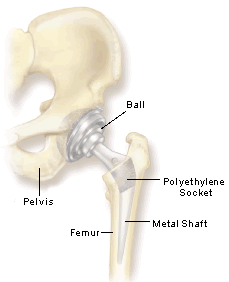
When arthritis strikes the hip joint, every step can bring stiffness and pain, restricting your activities -- both pleasurable and mundane. For many people in this situation, hip-replacement surgery is the answer. Replacing the damaged, arthritic joint with a new, artificial one helps many patients resume walking without pain and return to a level of activity they haven't enjoyed in years. In the United States, more than 260,000 people annually have hip-replacement surgery, also known as total joint replacement or arthroplasty. Most patients undergoing joint replacement typically have osteoarthritis, the type of arthritis that occurs from wear and tear on the skeleton as we get older. Osteoarthritis causes deterioration of the smooth, slippery cartilage that normally cushions the bones where they meet. In the hip, this deterioration occurs between the head of the femur (the long bone of the thigh) and the hip socket (actually a part of the pelvis called the acetabulum). As the cartilage degenerates, the normally smooth operation of the joint becomes slowed by friction. Eventually, so much cartilage wears away that bone rubs on bone, causing pain, inflammation, swelling and loss of mobility. When the pain and lack of mobility become severe enough, and other measures don't bring sufficient relief, it may be time for a total joint replacement. The procedure itself is quite straightforward. An orthopedic surgeon replaces the head of the femur with a prosthetic device composed of a metal or ceramic ball connected to a metal shaft. The shaft is inserted into a hole drilled into the thighbone. A polyethylene socket replaces the natural socket in the pelvic bone.
If you are considering hip replacement, what is the best way to prepare yourself for the surgery? -- The Editors The Physician's Perspective Dr. Robert Poss Patients and their doctors have a common goal in joint-replacement surgery -- to get the best outcome possible. But often their viewpoints on the procedure can be very different. For surgeons, the operation is an everyday occurrence, but it is likely an entirely new experience for the patient. Similarly, physicians may of necessity focus more on the surgery itself, while patients may be more focused on recovery and how they are going to cope once the new hip is in place. This study from the Mayo Clinic helps both patients and their doctors to better understand the concerns of people undergoing this procedure. In many cases, patients don't know which questions to ask prior to surgery. Or, they don't write them down and forget them when the time comes to meet with the surgeon. The study identifies specific questions and concerns that patients can discuss with their own doctor. As the top six concerns show, most people undergoing joint replacement primarily worry about the aftereffects of the surgery. Patients also expressed anxiety about blood transfusions, hip dislocation and one leg ending up longer than the other. All of these are valid issues that your doctor can address prior to surgery. For example, several methods are available to bypass the need for a transfusion. Although the blood supply today is extremely safe and the risk of contracting HIV or hepatitis C (another common fear) is very small, many people bank their own blood (called autodonation) before surgery to avoid getting a transfusion of someone else's blood. Most people have pain after the procedure while the tissues heal. Exercising the joint after surgery may also be painful until the surrounding muscles become stronger. The pain should ease with time. Usually within a day of your surgery, you will be out of bed and putting weight on the new hip joint. During your hospital stay, which typically lasts a few days to a week, a physical therapist will help you to exercise the hip and to learn how to manage everyday activities, such as putting on shoes or climbing stairs. Some patients spend a short time in a skilled nursing facility for additional rehabilitation after leaving the hospital and before returning home. It's important to discuss your home situation with your physician -- and physical therapist, if possible -- before the surgery so you can better prepare for your recovery. Do you live alone, or is there someone at home to help you? What potential hazards, such as stairs, does your home contain? What kind of physical therapy will be available after you've been discharged? Most hip-replacement patients can return to driving in about six weeks and by then also will be able to manage most day-to-day activities, such as walking. Within the first three months, you will be able to resume most other daily activities -- with the guidance of your doctor. Avail yourself of the printed information or pre-surgery classes about joint replacement that many hospitals offer. Some hospitals offer a team approach to patient education that allows you to meet with all the members of your health-care team, including physical therapists, before the surgery. This can be helpful for getting a well-rounded perspective on your surgery and recovery process. Also realize that a hip replacement is a long-term commitment -- it's important to see your doctor for X-rays within the year following surgery and then periodically over the life of the artificial joint (usually 10 years to 15 years). This allows your physician to detect any problems, such as loosening of the prosthesis, as early as possible. Overall, the best approach to hip replacement is to educate yourself and to ask questions so that there are no surprises. The chances of success are greatest when both the physician and patient understand one another's viewpoint. Dr. Robert Poss is a professor of orthopedic surgery at Harvard Medical School and vice chairman of the Department of Orthopedic Surgery at Brigham and Women's Hospital in Boston, Mass. For more information, send a business-sized, stamped self-addressed envelope to the American Academy of Orthopedic Surgeons, P.O. Box 2058, Des Plaines, IL 60017 for a free brochure on total joint replacement or see the group's Web site. |